Linda had been experiencing constant and bothersome dry, irritated eyes as well as eye fatigue for approximately 6 months and was finding that her symptoms were worsening in the afternoon, which prompted her visit. She found minimal to no relief with previous at-home therapies, including hot towel compresses, use of
over-the-counter lubricating eye drops (5x/day) and over-the-counter lubricating ointment (nightly use).
For background, Linda does not consume alcohol and is a non-smoker with no history of previous
refractive surgery or ocular trauma or injury. For over 2 years, she had taken Losartan 100mg (1x/day) to control her hypertension. In general, her best corrected visual acuity was 20/20 in each eye.
Diagnosing meibomian gland dysfunction
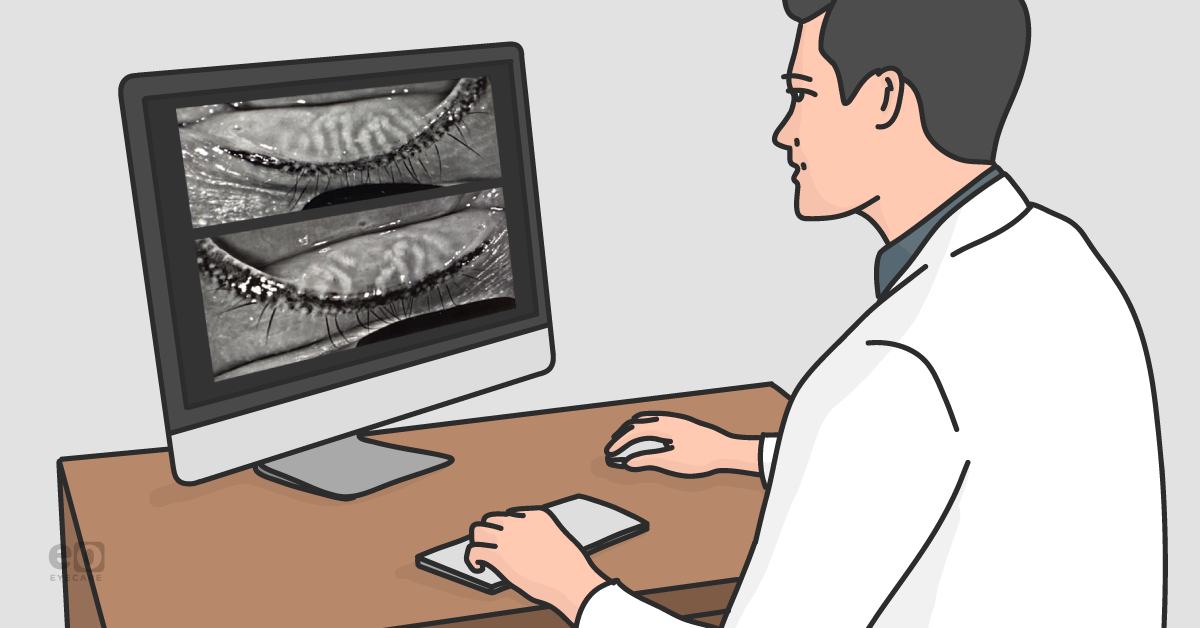
Image 1 illustrates lower eyelid with long-standing tattoo eyeliner and missing lashes (madarosis).
Image 1
Upon examination, I discovered that Linda had long-standing tattooed eyeliner, madarosis, toothpaste-like Meibomian gland expression, and mild lid wiper epitheliopathy (LWE). Her corneas were clear of any vital dye staining; however, she had a reduced tear breakup time (TBUT) of 5 seconds in each eye and had an abnormal score of 18/28 on the
Standard Patient Evaluation of Eye Dryness Questionnaire (SPEED). Her
Tear Osmolarity (TearLab) revealed normal values of 293 mOsms/L and 290 mOsms/L, in the right and left eye, respectively.
Image 2 illustrates lower eyelid manual expression post-
LipiFlow (1st visit)
Image 2
Using the
Keratograph 5M (Oculus), her tear meniscus height (aqueous) was reduced in the right eye and normal in the left eye. Linda’s non-invasive tear breakup time (NIKBUT) was moderately reduced in both eyes while her conjunctival injection was mild in both eyes.
Additionally, infrared imaging with meibography showed significant gland changes in both lower eyelids with her right lower eyelid graded as 1.5 out of 3 and her left lower eyelid with a grade of 2.2 out of 3. (Grading scale for MG structures: 0 = normal, 1 = mild changes, 2 = moderate changes, and 3 = severe change).
Image 3 shows meibography of the right lower eyelid.
Image 3
Image 4 shows meibography of the left lower eyelid.
Image 4
Image 5 demonstrates lower eyelid manual expression post-LipiFlow (2nd visit).
Image 5
Our treatment for MGD
Based on her examination results, it was discussed and determined that Linda would benefit from same-day treatment with 3 office-based treatments including LipiFlow,
Intense Pulse Light (IPL), and BlephEx.
- LipiFlow Thermal Pulsation System is an automated and cutting-edge device that simultaneously liquifies and unclogs poor meibum from the meibomian glands.
- BlephEx lid exfoliation removes excess bacteria, biofilm, and bacterial toxins especially at the opening of the meibomian glands.
- Intense Pulse Light (IPL) with OptiLight delivers gentle pulses of light at specific wavelengths to reduce inflammation, increase mitochondrial gland activity, preserve gland structure, and photo-sanitize bacteria and demodex.
At our practice, the typical order performed is BlephEx followed by IPL, finishing with LipiFlow. I start with BlephEx since it addresses the buildup and biofilm, then I move to IPL, which targets the inflammation, and lastly
apply LipiFlow to remove the obstruction.
For patients with moderate-to-severe symptoms and thick, abnormal meibum, I’ll often consider manual expression post-Lipiflow, as I’ve done in this case. If there’s a fair amount of abnormal meibum released to the surface during manual expression then I’ll repeat BlephEx.
Image 6 depicts the upper eyelid with long-standing tattoo eyeliner and mild lid wiper epitheliopathy (LWE).
Image 6
Although Linda began to feel gradual relief after her first visit, she chose to continue therapy every 4 weeks with the combination of LipiFlow, OptiLight, & BlephEx. Over the course of her visits, we slowly introduced and updated her home regimen to include iTear100 neuro-stimulation,
RegenerEyes Pro,
Avenova, and PRN DE 3.
Within 4 months, her eyes felt much better with both signs and symptoms improving! They were less gritty, LWE resolved and her gland expression was healthier with cloudy to clear meibum (oils) instead of the toothpaste-like oils. In comparison to her SPEED assessment from June 2021, Linda’s score improved significantly to an 8/28 (down from 18/28).
Key Takeaways:
- Interestingly, her glands benefited from manual expression post-LipiFlow.
- Despite her eyelid tattoos, we safely and effectively performed multiple treatments of LipiFlow, BlephEx, and OptiLight.
- Even though her tear osmolarity was normal, other objective findings were abnormal such as TBUT, NIKBUT, meibography, gland expression, etc.
- It is important to note that she had significant gland atrophy, yet she still improved from in-office MGD treatments.
In conclusion
Remember managing patient expectations is paramount. Reassure them of the following:
- It may take weeks to months to experience a breakthrough.
- We may make adjustments along the journey.
- We’ll strive to reduce the frequency and severity of flare-ups—ideally, leading to more good days than bad.