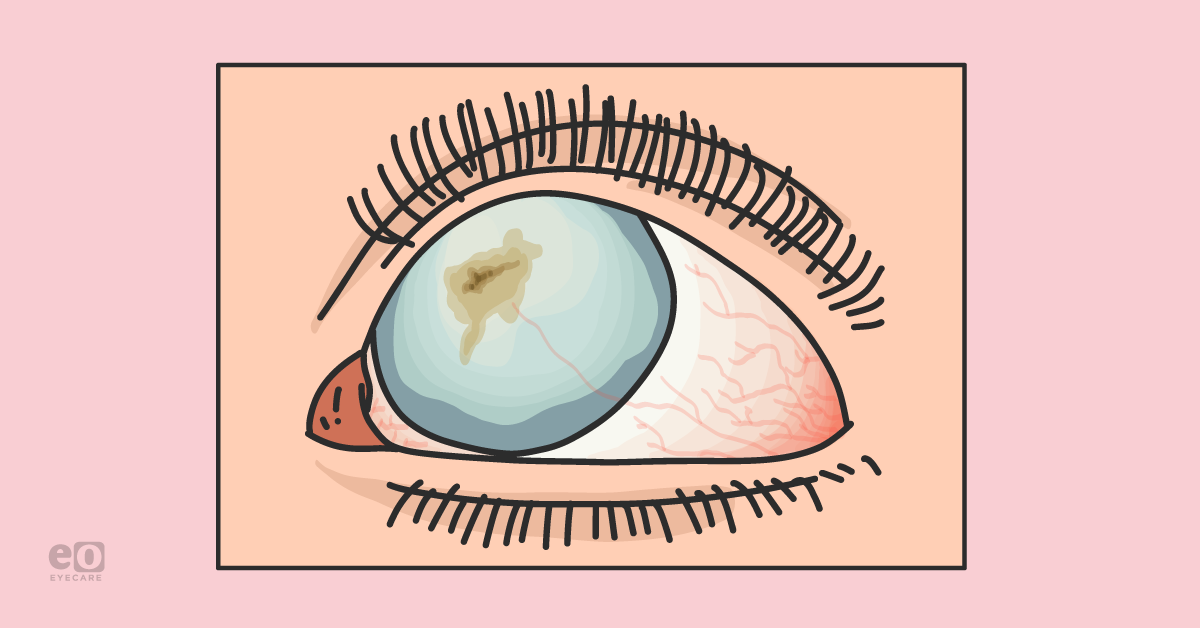
The
cornea is a very unique part of our eyes. A key histological feature of the cornea is the specific pattern of collagen within the stroma and its avascularity, which give the cornea its unique transparency and the capacity to focus light on the retina.
Changes to collagen that can lead to “corneal leukoma” or corneal scarring:1
- Type
- Size
- Distribution
- Inflammation
- Spatial organization due to infection
- Any other cause of opacity and irregularities
The cornea covers the pupil, iris, and anterior chamber. If a scar is peripheral, or even paracentral, it may not alter the vision at all. However, if the scar is centrally located it may cause a significant loss of vision.
Layers of the Cornea
1) Epithelium
- Barrier to microbes, chemicals, and water
2) Bowman’s layer
3) Stroma
- Mechanical Strength
- Transparency
4) Descemet’s membrane
- Basement membrane anterior to endothelial cells
5) Endothelium
- Responsible for the transparency of the cornea by regulating the stromal water content (“water pumps”)2
Causes of corneal scarring
- Severe dry eye
- Injury or trauma (idiopathic, chemical, and surgical)
- Infections
- Diseases of the cornea or eye surfaces, such as keratoconus
Symptoms of corneal scarring
The typical symptoms of corneal scarring are blurred vision, light sensitivity, pain, and foreign body sensation. Corneal scarring often presents as a complication of another condition; therefore, it usually presents as a change in the signs and symptoms of these preexisting conditions, mainly a change in the visual acuity.
For example: keratoconus is usually a bilateral disease, however if there are complications caused by corneal scarring, patients may present with asymmetric symptoms such as one eye may be much more severely blurred than the other.4
Diagnosis of corneal scarring
The vast majority of corneal scars and their underlying causes can be easily diagnosed during a routine slit lamp exam. Corneal scarring has a characteristic white opacity and an associated loss of the normal clarity of the cornea. Sometimes, corneal scars are easy to detect with just a pocket flashlight.
Anterior scars may or may not alter
corneal topography; they may also simply create a haze, leading to reduced visual acuity. Corneal topography and anterior segment OCT can help delineate the extent of scarring and also aid in surgical planning.
Treatment options
Patients with severe vision loss due to central corneal scars can benefit from visual rehabilitation. For mild scars, the refractive error from the scar may be corrected with glasses or contact lenses (soft, scleral, and rigid gas permeable lenses are options).
In some cases of anterior scars, mainly involving the Bowman’s layer and the anterior stroma, a superficial keratectomy (SK) may be performed.4 Here, a lamellar resection of the diseased cornea is removed manually and a bandage contact lens is placed to allow for healing.
In some severe cases of corneal scarring, neither glasses nor contact lenses can improve vision. In these situations, a corneal transplant can be considered.
Over the last few decades
corneal transplantation techniques have rapidly expanded from the traditional full thickness penetrating keratoplasty (PKP) towards selective lamellar keratoplasty to only remove the diseased layers of the cornea.
5Full thickness keratoplasty was the most common corneal transplantation technique over the last few decades, however, the popularity of selective lamellar transplantations of the affected layers of the cornea is increasing.
If the scar is relatively superficial, deep anterior lamellar keratoplasty (DALK) may be attempted.6 Otherwise, a traditional full thickness penetrating keratoplasty may be performed.7
Common types of corneal transplantations:
| Name | Technique | Indication | Complications |
|---|
| Penetrating Keratoplasty (PKP) | Removal of all layers of the host cornea with full thickness transplantation of the donor graft. | Full-thickness scar, bullous keratopathy, keratoconus, graft failure. | Graft rejection, graft failure, hemorrhage, infection, astigmatism, suture complications. |
| Deep Anterior Lamellar Keratoplasty (DALK) | Diseased host epithelium and stroma removed. Transplant of donor cornea epithelium, Bowman’s membrane, and corneal stroma. | Keratoconus, stromal scar, hereditary stromal dystrophies. | Graft rejection, intraoperative Descemet membrane tear, astigmatism. |
| Descemet Stripping Automated Endothelial Keratoplasty (DSAEK) | Both endothelium and Descemet membrane are removed and replaced with the donor endothelium, Descemet membrane and stroma. | Fuchs’ dystrophy, bullous keratopathy, graft failure. | Graft detachment, graft failure, graft rejection. |
| Descemet membrane endothelial keratoplasty (DMEK) | Both endothelium and Descemet membrane are removed and replaced with the donor endothelium and Descemet membrane. | Fuchs’ dystrophy, bullous keratopathy, graft failure. | Graft detachment, graft failure.8,9 |
|
Visual rehabilitation
In cases where vision cannot be rehabilitated (usually this happens when there is irreversible damage to other intraocular structures, or if the patient cannot undergo surgery to correct their condition), low vision therapy may be of significant help. The goal of low vision rehabilitation is to train patients in strategies of coping with the diminished vision. Maintaining independence and improving the quality of life are the main objectives.
There are several options available with low vision programs; usually after assessment of vision, there are suggestions made for environmental modifications, introduction to assistive devices, and training.8
All state governments in the United States fund agencies to provide visual rehabilitation services. These agencies take care of most of the rehabilitative efforts, either directly or through subcontractors. Two examples of trusted low vision resources for patients are
Helen Keller Services for the Blind and the
Lighthouse Guild.
9Conclusion
Corneal scarring can be due to trauma, infections, ulceration, corneal dystrophies, or other diseases that may cause significant vision impairment. Management of the scarring depends on different factors including the histological location of the scar within the corneal tissue, the availability of corneal transplants, and the visual rehabilitation services.