Orthokeratology is a viable option for treating refractive error, offering a safe and effective solution for providing vision correction to patients during their waking hours while improving quality of life.
1-4 Orthokeratology has been shown to be effective in
managing the progression of myopia.
5The
prevalence of myopia is increasing worldwide and progressing to even higher degrees than before.
6,7 This will only increase the risk of sight threatening complications that can lead to blindness in adulthood,
8,9 like myopic macular degeneration, which we know increases 67% with each diopter increase in myopia.
10Now armed with the opportunity to
slow the progression of myopia rather than simply correct vision, it is more important than ever before for eyecare professionals to become equipped and be prepared to manage myopia by leveraging the various treatments and tools available—including orthokeratology.
As myopia management grows in importance in eyecare and the public eye, optometrists may find themselves increasingly called upon to provide this service to their patients. Although orthokeratology has been a well-known aspect of myopia management for several years, the recent FDA approval of
Johnson & Johnson Vision’s ACUVUE Abiliti Overnight Therapeutic Lenses for the management of myopia will undoubtedly contribute to the growing demand for orthokeratology in eyecare practice as your patients—and more importantly, their parents—become more aware of this treatment option and its utility.
For eyecare professionals to incorporate orthokeratology into practice, it is important to understand the basics of orthokeratology, mechanisms, and some common myths.
MANAGING MYOPIA: A CLINICAL RESPONSE TO THE GROWING EPIDEMIC
Intended to provide guidance to eyecare practitioners in the management of myopia in clinical practice, this guide has been created in collaboration with the American Optometric Association, the Singapore Optometric Association, the American Academy of Optometry, and Johnson & Johnson Vision and is informed by currently available scientific research.
Orthokeratology mechanism
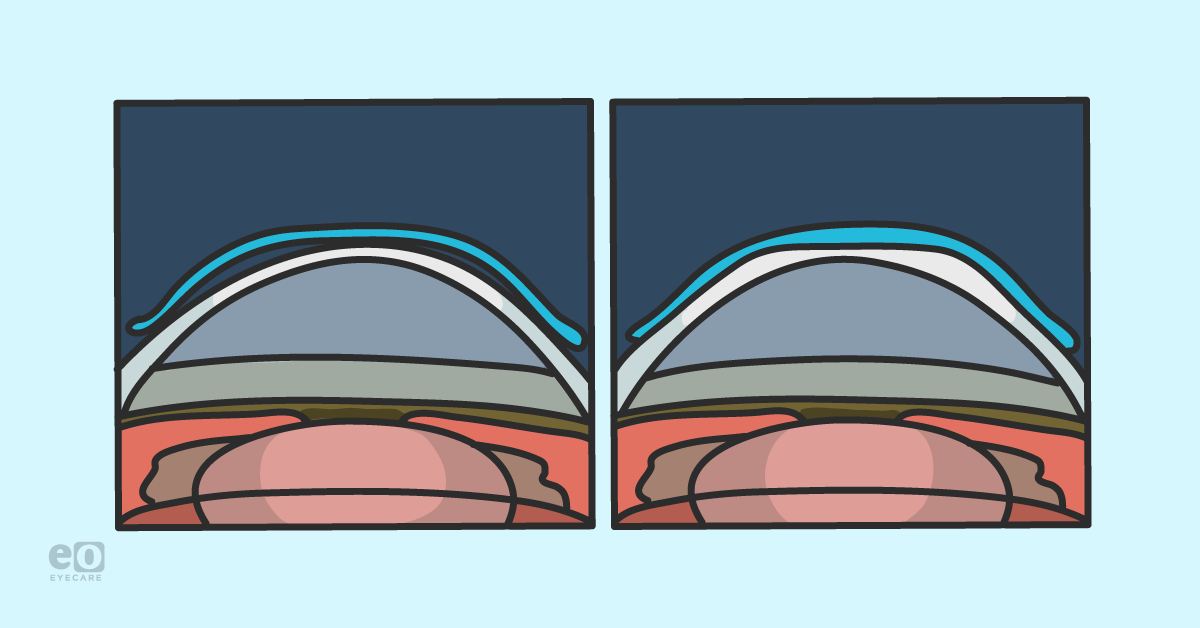
Orthokeratology lenses for correction of myopia functions by causing a flattening of the central cornea and a steepening of the mid-peripheral cornea, which is accompanied by reversible changes to the corneal epithelial and stromal layers.11-13 The mechanism that elicits the morphological change is somewhat less understood.
A variety of theories have been proposed, including epithelial cell redistribution with migration of epithelial cells to the midperiphery, with another theory suggesting compression or remodeling of epithelial cells due to changing pressure or forces that does not require migration.14,15 Current thought is that orthokeratology treatment is achieved as a result of hydraulic forces beneath the contact lens, with a properly fit lens forming a semi-closed fluid/tear reservoir inside the alignment zone of the lens inducing the change in corneal shape.16, 17
Orthokeratology Design
Orthokeratology lenses feature a reverse geometry design consisting of several different zones or curves. These curves can be modified independently to provide the best fit and comfort for patients.
Image 1, below, depicts the anatomy of an orthokeratology lens.
Image 1
Base Curve (BC) / Back Optic Zone Radius (BOZ)
The base curve is the central portion of the lens. It is typically chosen based upon the refractive error of the patient and the amount of correction desired and is typically between 5.0mm and 6.8mm in diameter.18
Reverse Curve
The reverse curve functions to control apical clearance and impacts lens centration as a result. One of the primary functions of the reverse curve is to raise or lower the BC / BOZR to create the desired amount of apical clearance. This zone is typically between 0.5mm to 1.0mm wide and is steeper than its neighboring curves. The tear film reservoir is a function of the clearance under this curve, which is impacted by myopic correction.18
Often the BOZR/BC and reverse curve are adjusted in conjunction with one another to affect the overall lens sag (lens clearance over the cornea). This inherently determines how much treatment is given to the patient.
Alignment Curve
This curve most impacts centration and is typically 0.5mm to 1.0mm wide. The lower the eccentricity, the steeper the alignment curve needs to be to provide alignment.18
Peripheral Curve
This curve controls the amount of edge lift at the peripheral cornea and commonly has a width of 0.2mm to 0.5mm.18
Now that we have established the basics of orthokeratology lens design and mechanism, it is critical to examine and debunk some common myths.
We created a handy guide that summarizes the most common myths surrounding ortho-k lenses! Check out the infographic below!
Myth One: Orthokeratology lens fitting is too complicated
In the past, orthokeratology lens fitting was complicated and required diagnostic fitting. While there were some benefits of having a fit set on hand, the process was also highly subjective and inexperienced fitters would be prone to more lens reorders and lower success rates. The tools and technology needed to precisely measure the corneal surface and manufacture lenses to fit it were not readily available. However, technology has advanced, as has our understanding of orthokeratology. Most companies have experienced fitting consultants that can help design the lens and answer any questions you have, making the process easy for any eyecare practitioner.
Fitting methods like topography-based empirical fitting has given eyecare professionals a more accessible entry point into fitting orthokeratology lenses as it requires less experience and expertise in order to get started.
A closer look at empirical fitting as a user-friendly way of fitting orthokeratology lenses
Most view empirical fitting as the easiest, most user-friendly method to fit orthokeratology (also known as ortho-k) lenses. While corneal topography remains the gold standard for ortho-k fittings, many eyecare practitioners experience success with keratometry readings, spectacle Rx, and horizontal visible iris diameter (HVID) measurements.
Providing topography-based data to the company can help reduce the number of refits since this data provides more information and perhaps a better understanding for the consultants as to how the lens is sitting on the eye (centered or off-axis), and whether there is an adequate treatment effect.
As a practitioner, you want to try to limit the number of follow-ups, otherwise it becomes a burden for the patient and parent. The follow-ups can be time consuming for the practitioner and patient since each visit usually requires topography, autorefractor, visual acuity and slit-lamp examination.
Though this type of fitting tends to be the easiest, the fitter tends to have less control over the lens design. Empirical fitting is only as successful as the quality of the data you provide. So long as you provide the company with precise measurements detailed above, including an accurate refraction with and without cycloplegia, less time and money will be spent on follow-ups and remakes meaning your patients and parents will have a positive experience, which also means less chair time, which is also good for your practice.
Providing a good quality topography image
The first step to utilizing topography to analyze the fit of the lens is to take the best quality image possible. When capturing a topographic image, the lid should be held out of the way as best as possible. Sometimes the patient is able to hold their eyes open enough to capture the entire cornea, other times a technician is needed to hold the lids back with a Q-tip.
However, it is also important to try to capture the image with a stable tear film. This can be difficult if the patient has dry eyes or the eyes are opened too long before the photo. Have the patient blink two times and then tell them to open as wide as possible. You should also have the machine lined up as centrally as possible before they blink and then reposition the machine as quickly as possible and capture the image. Sometimes use of artificial tears or proparacaine can help stabilize the tear film but should only be used as a last resort.
Capturing a strong baseline scan is crucial for comparison of treatment maps moving forward.
Other ways corneal topography is useful for orthokeratology success
Empirical fitting from a few data points (keratometry, refraction, HVID) is very simple, but more difficult to troubleshoot. Corneal topographers can provide extremely detailed information about the entire ocular surface, which can be paramount when starting the lens design process. Highlighted below are some of the key data points and measurements of corneal topography leveraged in the fitting process.
Axial, tangential, and differential mapping
Axial, or power, maps give us data about the type of corneal astigmatism and power of the corneal curvature. These are the most helpful maps when designing custom lenses.19
Tangential maps allow us to see curvature of the cornea in one place, relative to neighboring tangential points. This is most helpful when analyzing topography for lens concentration.19
Difference maps are used to compare a treatment map to the baseline scan and can be used to show the position of the lens more clearly. When comparing the post treatment tangential map to the baseline, it is easier to see the position of the lens in the closed eye environment.
Evaluating orthokeratology treatment
A lot of the headache of trial and error of fitting multiple orthokeratology lenses has been done away with. Companies have made it easy for inexperienced and experienced practitioners to fit these lenses. As stated before, many of these companies have experienced consultants to help make the design decisions for you. Just email them your data (topography without lenses, autorefractor with and without lenses, visual acuity with and without lenses and pictures of the lens on the eyes with
fluorescein dye and cobalt blue filter) and they will let you know the new lens parameters and send them to your office.
Other software programs allow slightly more experienced practitioners to perform a “mock trial” of the lenses by inputting the lens parameter changes into the software and viewing how it would change the fit and treatment of the patient’s eye.
Lens centration along the visual axis during the night is crucial for optimal treatment effect and to limit aberrations or distortion.
Make sure to confirm both the patient and parent have a full understanding of the procedure and that orthokeratology use occurs under parental supervision only.
The practitioner should be able to evaluate the lens fit on the eye, which is not overly difficult. It is helpful to use a Wratten filter with cobalt blue light. A bullseye fluorescein pattern of central bearing, mid-peripheral pooling, and adequate edge lift should be observed. As with all gas permeable lenses, centration and movement should also be assessed. Minimal movement of ≤1 mm is ideal with centration both vertically and horizontally.
Image 2 illustrates a right eye showing ideal fit with bullseye pattern visible with fluorescein staining.
Image 2: Contributed by Laura Goldberg, OD.
If using a topographer, it is also a good idea to have a basic understanding of some of the common issues that can arise with lens fitting and how it would impact the topography images.
Myth two: Orthokeratology is risky
For a lot of practitioners, safety of orthokeratology is a concern. The thought of putting a lens on a child and sending them to bed can be scary, but let’s review some key considerations.
Infection
Rates of microbial keratitis have been reported to be approximately 7.7 cases per 10,000 patient years.
20 In other words, of 100 patients in lenses, on average, one case of microbial keratitis every 13 years was expected. However, new data suggest that the incidence of microbial keratitis in children wearing overnight orthokeratology is lower than previous studies suggest and is similar to rates associated with use of daily wear soft contact lenses.
21 Many of the acanthamoeba cases that were being reported were in countries that had inadequate regulation for orthokeratology. Additionally, most of the adverse cases reported resulted from improper care of lenses, including exposure to tap water. When compared with other contact lens modalities, rates of
microbial keratitis in orthokeratology wearers are similar to those of overnight
soft lens wearers.
2,22Hypoxia
Another sticking point for some is oxygen transmissibility. Fortunately, this has become a non-factor as a result of an increase in materials with Dk values at or above 100. While there is a slight increase in mid-peripheral corneal swelling (2% to 6%), when the lenses are first worn overnight, overall corneal swelling is similar to that of non-lens wearing eyes after 30 days of use.3,23 Most proprietary lens designs are in high Dk materials by default. Those planning on custom designing lenses should specify the material they are manufactured in.
Long term corneal changes
At this point, the eyecare industry has a good handle on the short term (<1 year) effects of orthokeratology, but simply doesn’t have large amounts of data on those patients wearing orthokeratology lenses for >10 years. Some anecdotal evidence shows that, provided a lens is fit properly, there are no detrimental changes (such as permanent corneal warpage) in patients wearing lenses for over a decade.
The amount of time it takes to recover calls into question the assumption that orthokeratology is an epithelial phenomenon. The entire corneal epithelium regenerates in 7-10 days.24 If it were only the epithelium that changed after orthokeratology wear, the cornea should completely return to its pretreatment shape after those 7-10 days. A possible explanation for this discrepancy in recovery time may be due to changes to the Bowman’s membrane and central stroma. There is evidence that both layers undergo change during orthokeratology wear and effects can persist long after lens wear has been discontinued. One study suggests the changes to Bowman’s may be irreversible.25 That said, none of the changes caused a reduction in vision and refractive error does stabilize.
Myth three: Fitting orthokeratology isn’t worth the time and effort
Understanding return on investment begins with looking at costs and revenue potential, and this is no different for orthokeratology than any other eyecare specialty, treatment, or offering. If the appropriate time and resources are invested upfront to implement a system to fit the lenses effectively, orthokeratology can be a great use of chair time. Just like any other specialty you choose to offer, you have to invest up front to ensure it goes smoothly.
The costs include equipment, such as an autorefractor (which most practices already have) and a topographer, which can be obtained at a reasonable cost. There is no need for a lens fitting kit, particularly if you wish to fit lenses empirically.
These patients frequently become patients for life, since they trust the practitioner and their specialty skills. Word of mouth can travel fast and bring more patients to a practice.
Building a specialty practice can ensure a practice is successful for many years to come and allow it to become less reliant on insurance-driven exams.
Myth four: Patients aren’t interested in orthokeratology
While many parents are unaware of the risks and complications connected to high myopia, when given the information, they are eager to combat the problem. When choosing myopia management, safety, efficacy, complications, cost, and time are their prime considerations. And when offered orthokeratology as an option, a significant number of patients will choose it over other options, including
multifocal contact lenses, bifocal spectacles, undercorrection, and pharmaceutical eye drops.
26Gain a comprehensive knowledge of orthokeratology
Naturally, it is the role of the doctor and staff to educate patients on the benefits, risks, and process of orthokeratology. An explanation of orthokeratology should be as natural as an explanation of cataracts. Highlights should include myopia management effects and convenience. Nailing your scripts will make the flow during the consult and fitting process much more consistent and schedule-friendly.
Educate your staff
The two-edged sword of orthokeratology (and most contact lenses in general) is that the success or failure of the specialty is often dependent on the staff. The evaluation of a lens on the eye or a topography is a very quick process. It is the education, insertion/ removal training, and initial work up that consumes the majority of the visit. So, if 90% of the visit is in the hands of your staff, your focus should be on developing their skills. They should be just as knowledgeable on the information concerning myopia, how the lenses work, and (especially) care of the lenses. If done correctly, you should be the enforcer of the information presented by the staff, not the primary source.
Clear communication
Communication is a major factor in success when it comes to fitting orthokeratology lenses. Many patients are not familiar with this technology; therefore, it is essential to effectively communicate every detail of the process. In a few sentences, one can address what orthokeratology is, how it works, and what the benefits to the patient are from a convenience, monetary, and ocular health standpoint. Think about it as a 30-second elevator speech. Next, give them more detailed information in print and ask when they would like to schedule a consultation.
The benefits of a separate consultation
Often, the parent is the most critical player for the initial decision, but the patient will determine the long-term success. Parents have to feel comfortable from both a psychological standpoint and a monetary one. They need to feel that orthokeratology is one of the best options for their child and believe it is well worth the price. There are a couple of steps in helping parents understand the benefits. First,
start the conversation.
Know that an initial consultation is necessary. A person doesn't go to the dentist for a cleaning, find out they need braces, and get them put on in the same visit. So why try to do a full exam and orthokeratology fitting in a single day? Though it’s often true that lenses could be fitted just with the information gained in the patient’s initial visit, the real purpose of the consultation is to guarantee buy-in.
The consultation gives parents and patients time after the initial presentation of the concept of orthokeratology to think about it and do some self-directed learning. Letting parents spend time looking up information prior to coming in for the meeting builds a huge amount of trust, but be prepared to answer all the questions they have.
Once their fears are allayed, discuss all the details, such as pricing, visit schedule, lens warranty information, etc. Spending a little extra time up front and being totally explicit about your practice’s orthokeratology services will save an exponential amount of time and money in the long run.
Regardless of how consults and education are structured, the most important thing is a belief in the modality. The most well written script is worthless in the hands of an individual who doesn’t believe that orthokeratology is a good option. The practitioner must buy in before they can expect their patients to do so.
Myth five: Orthokeratology lenses are perpetually painful
It is true that orthokeratology lenses are uncomfortable at first; however, they don’t hurt continually. Though a person won't forget they are wearing orthokeratology lenses, like they might with a daily disposable soft lens, the discomfort is greatly reduced as the patient becomes acclimated.
Have the patient close their eyes. Almost all sensation created by a GP lens is a result of lid/lens interaction. The times the lens is most uncomfortable is during the blink. If the lids are shut, the lens is static. Instantly, the lens becomes more comfortable. Reminding the patient that their eyes will be closed 98% of the time when they wear orthokeratology lenses is a powerful way to overcome issues with initial comfort.
Myth six: Insertion and removal of orthokeratology lenses is too difficult for young children
Though teaching children as young as 7 years old to handle and care for lenses is not an easy task, with proper instruction and parent participation, it can be effectively accomplished.
Insertion and removal (A&R) training starts not at the dispensing visit, but at the consultation. When all the details have been worked out and contracts signed, give the patient and parent some homework. The homework consists of the patient practicing touching their own eyes for five minutes per day, every day, before returning to the office for the dispensing visit.
If patients are able to master lid manipulation and touching the conjunctiva, insertion at the office is much easier for all involved. The only difference when applying an actual lens will be that the patient looks in the mirror and applies the lens directly to their cornea. This is relatively easy to teach.
Removal is an entirely separate process. Ideally, patients should be able to remove their orthokeratology lenses with no accessories, which is why many practitioners refuse to give children plungers to avoid the risk of injury. However, the practitioners will use the plungers as the primary method of removal. Practitioners can choose which camp they fall into.
Again, it’s critical that both the patient and the parents understand how to perform both insertion and removal to reduce the chance of failure when getting orthokeratology lenses in and out. With a number of different strategies at hand, it’s very rare to find a case where someone totally fails the insertion or removal. But, if it does happen, have the patient and parent practice touching their eyes at home for another period of time before doing the real insertion and removal training.
With proper training and practice, even elementary-age children can learn to safely apply and remove lenses. Therefore, fear should not dissuade the prescription and use of orthokeratology in young patients.
Orthokeratology presents a major opportunity for eyecare practitioners
In the past, orthokeratology could largely be considered a “fringe” vision-correcting technique, but as research on myopia development and progression continues to evolve, orthokeratology may soon become a staple for the eyecare practice.
Financials aside, offering orthokeratology and other myopia management options is truly in the best interest of young patients. The first step in becoming an orthokeratology fitter is personally buying in. One will never be successful if they don't believe in it. Some manufacturers will provide lenses to enable a practitioner to try them out for themselves or on a staff member. The effect is powerful. Orthokeratology lenses provide another tool in a practice’s toolbox and make for more outstanding clinicians.
Sources:
- Lipson MJ, Sugar A, Musch DC. Overnight corneal reshaping versus soft disposable contact lenses: Vision-related quality-of-life differences from a randomized clinical trial. Optom Vis Sci 2005;82:886–891.
- Hiraoka T, Okamoto C, Ishii Y, et al. Patient satisfaction and clinical outcomes after overnight orthokeratology. Optom Vis Sci 2009;86:875–882.
- Queiros A, Villa-Collar C, Gutiérrez AR, et al. Quality of life of myopic subjects with different methods of visual correction using the NEI RQL-42 questionnaire. Eye Contact Lens 2012;38:116–121.
- Santodomingo-Rubido J, Villa-Collar C, Gilmartin B, et al. Myopia control with orthokeratology contact lenses in Spain: A comparison of vision related quality-of-life measures between orthokeratology contact lenses and single-vision spectacles. Eye Contact Lens 2013;39:153–157.
- Huang J, Wen D, Wang Q, et al. Efficacy comparison of 16 interventions for myopia control in children. Ophthalmology 2016;123:697–708.
- Vitale S, Sperduto RD, Ferris FL III. Increased prevalence of myopia in the United States between 1971–1972 and 1999–2004. Arch Ophthalmol 2009; 127:1632–1639.
- Holden BA, Jong M, Davis S, et al. Nearly 1 billion myopes at risk of myopia-related sight-threatening conditions by 2050—Time to act now. Clin Exp Optom 2015;98:491–493.
- Perkins ES. Morbidity from Myopia. Sight Sav Rev 1979;49:11-9.
- Flitcroft DI. The Complex Interactions of Retinal, Optical and Environmental Factors in Myopia Aetiology. Prog Retin Eye Res 2012;31:622-60.
- Bullimore MA, Brennan NA. Myopia Control: Why Each Diopter Matters. Optom Vis Sci 2019;96:463-5.
- Swarbrick HA, Wong G, O’Leary DJ. Corneal response to OrthoKeratology. Optom Vis Sci 1998;75:791–799.
- Tsukiyama J, Miyamoto Y, Higaki S, et al. Changes in the anterior and posterior radii of the corneal curvature and anterior chamber depth by orthokeratology. Eye Contact Lens 2008; 34:17–20.
- Chen R, Mao X, Jiang J, et al. The relationship between corneal biomechanics and anterior segment parameters in the early study of orthokeratology: A pilot study. Medicine 2017;96:1–6.
- Choo J, Caroline P, Harlin P. “How does the cornea change under corneal reshaping contact lenses?” Eye Contact Lens 2004;30:211–213.
- Choo JD, Caroline P, Harlin P, et al. Morphologic changes in cat epithelium following continuous wear of orthokeratology lenses: A pilot study. Cont Lens Anterior Eye 2008;31:29–37.
- Coon LJ. Orthokeratology, Part 1: Historical perspective. J Am Optom Assoc 1982; 53: 187–195.
- Vincent SJ, Cho P, Chan KY, Fadel D, Ghorbani-Mojarrad N, González-Méijome JM, Johnson L, Kang P, Michaud L, Simard P, Jones L. CLEAR - Orthokeratology. Cont Lens Anterior Eye. 2021 Apr;44(2):240-269.
- Korszen E, Caroline, P. The Anatomy Of A Modern Orthokeratology Lens. Contact Lens Spectrum. March 1, 2017. https://www.clspectrum.com/issues/2017/march-2017/the-anatomy-of-a-modern-orthokeratology-lens
- Gidosh, Nicholas. Six Topography Tips to Improve Your Orthokeratology Fitting Success. Contact Lens Spectrum. August 2020. https://www.clspectrum.com/newsletters/orthokeratology-in-practice/august-2020
- Bullimore MA, Sinnott LT, Jones-Jordan LA. The risk of microbial keratitis with overnight corneal reshaping lenses. Optom Vis Sci 2013;90:937–44.
- Bullimore MA, Mirsayafov DS, Khurai AR, Kononov LB, Asatrian SP, Shmakov AN, Richdale K, Gorev VV. Pediatric Microbial Keratitis With Overnight Orthokeratology in Russia. Eye Contact Lens. 2021 Jul 1;47(7):420-425.
- Liu YM, Xie P. The Safety of Orthokeratology–A Systematic Review. Eye Contact Lens 2016;42:35–42.
- Alharbi A, La Hood D, Swarbrick HA. Overnight orthokeratology lens wear can inhibit the central stromal edema response. Invest Ophthalmol Vis Sci 2005;46:2334–40.
- Remington LA. Chapter 2 – Cornea and Sclera. In: Clinical Anatomy and Physiology of the Visual System. Vol ; 2012:10–39.
- Nieto-Bona A, González-Mesa A, Nieto-Bona MP, Villa-Collar C, Lorente-Velázquez A. Long-term changes in corneal morphology induced by overnight orthokeratology. Curr Eye Res 2011;36:895–904.
- Cheung S, Lam C, Cho P. Parents' knowledge and perspective of optical methods for myopia control in children. Optom Vis Science. 2014 Jun; 91(6):634-41.