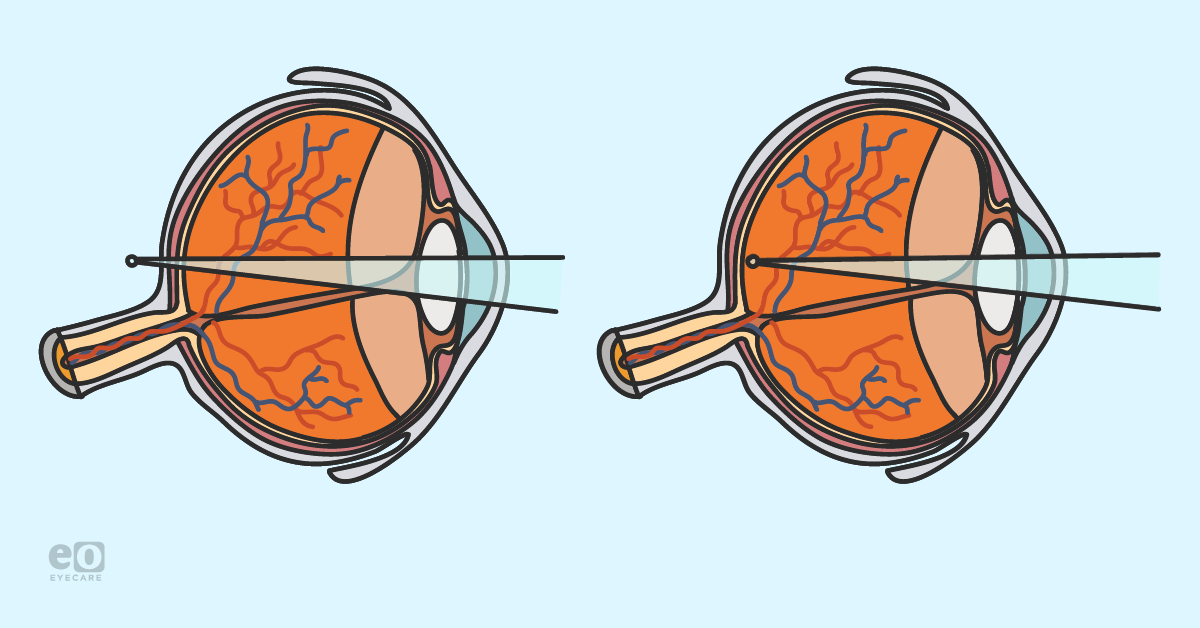
Prescribing for hyperopia can be challenging at times because there are no hard and fast rules. There are factors that need to be taken into consideration when determining the best correction. My residency in
binocular vision exposed me to many variations of hyperopic refractive errors and I’ve therefore developed my own system to create the most appropriate prescription. This article shares my personal reasoning behind prescribing for hyperopia and tips for creating a prescription for your patients!
For all patients, the initial element to consider for a full or partial Rx is the presence of a refractive amblyogenic risk factor.
Patients are at a great risk of developing hyperopic refractive amblyopia in the presence of:
- Anisometropia of +1.00 D or greater between both eyes
- Isometropia of +5.00 D or greater in each eye
I would consider pushing plus in these scenarios in order for the patient to achieve the best visual acuity possible.
In the absence of amblyogenic risk factors, I typically consider hyperopia of +3.00 D or greater to be significant to which an Rx of some sort will likely always be prescribed. It becomes tricky when the patient has mild to moderate hyperopia less than this value.
Consider obtaining a baseline 1% cyclopentolate refraction on the first exam for all infants, toddlers, and school-aged children to rule out any latent component and for future comparison if there are changes to the dry refraction over time.
Children from infancy to 10-years-old
Newborn infants have an average of +2.00 D of hyperopia. I typically wouldn’t provide a correction for hyperopia less than +3.00 D if the infant does not experience symptoms, has good VA and stereo, and absence of strabismus. We can carefully monitor these patients without treatment as emmetropization often leads to a reduction of hyperopia by 5-years-old. As you monitor, ensure that an esotropia or accommodative dysfunction does not develop later on.
Infants and toddlers with hyperopia of +3.00 D or greater are likely to remain hyperopic after emmetropization. Therefore, an Rx would be beneficial especially if other signs appear, including:
- Refractive amblyogenic risk factors
- Poor visual acuity or stereopsis
- An eso deviation
- Accommodative insufficiency or excess
- Convergence excess
Be aware that prescribing the full amount of hyperopia for an infant can interrupt the emmetropization process.
It may be best to prescribe a partial amount. If your
infant or toddler patient demonstrates hyperopia significantly greater than +3.00 D or a fully accommodative esotropia at any stage, these are situations where the full cycloplegic refraction could be prescribed.
After a few years, your patient has finally reached a school age where their near demands have increased. It’s time to repeat binocular vision testing and strongly consider an Rx for hyperopia less than +3.00 D if the patient appears symptomatic for:
- Blurred vision
- Asthenopia
- Accommodative dysfunction
- Esotropia
- Convergence excess
Most of these situations above require at least a partial Rx. When considering a partial Rx, I highly recommend cutting back only up to 1.50 D equally in each eye from the cycloplegic refraction.
The amount of plus that you cut back all depends on how many visual problems your patient experiences, and what their visual demands are at that age.
For younger children with minor symptoms and a low demand for near tasks, you can cut back on more plus power. For a patient with significantly symptomatic accommodative dysfunction, it would be best to provide a higher amount of plus to provide relief. There is no right or wrong way to prescribe as long as you trial in-office and understand the reason why you are prescribing that amount.
Younger children generally adapt very well to new prescriptions, even if they are high powered lenses. If you feel that your patient will benefit from the full hyperopic Rx, go for it! You’ll often be surprised at how quickly your patient will accept the new lenses. An alternative to prescribing glasses is to recommend contact lens wear to increase compliance and reduce aniseikonia.
You should also recommend
vision therapy in order to treat any accommodative or binocular disorder which may reduce the patient’s need for an Rx in general.
Adults and children older than 10 years
Consider providing a partial Rx for near tasks if patients with hyperopia less than +3.00 D experience symptoms of accommodative or binocular dysfunction. You may also
consider vision therapy as an alternative treatment option.
Sometimes I come into a situation where a teenager can accommodate through +3.00 D or more of uncorrected hyperopia and be completely asymptomatic. For patients like this, I monitor without treatment, educate on potential future symptoms and prime them for the possibility of needing glasses if those symptoms occur.
Teenagers and adults have a difficult time adapting to high powered plus lenses or significant changes in their previous prescriptions.
If you feel that your patient needs a higher hyperopic prescription, consider dispensing the glasses right after a cycloplegic dilation and advise them to wear the glasses for the rest of the day.
This gives the patient time to slowly adapt to the new lenses and feel more comfortable in them the next day!
Pre-presbyopic adults 30 to 40-years-old
Hyperopic adults can be challenging to prescribe for when they reach closer to the
presbyopic age.
Consider prescribing a partial distance correction that can be worn full-time in order to relieve their near visual symptoms.
An alternative option is to educate them on the need for a reading Rx sooner than expected. Lastly, contact lenses are a great method of correction for these patients especially if they have never worn glasses before.
Hopefully these suggestions give you a better understanding of when and how to prescribe for your low to moderate hyperopic patients. The more patients you see and manage, the more experienced you’ll feel in prescribing for hyperopia!