In the initial phases of the development of the surgical microscope, emphasis was placed on improving visualization.1-4 However, as time went on, concerns of phototoxicity surfaced.1-5 Attempts have been made to decrease the risk of microscope-light induced toxicity by a number of means (filtering illumination by corneal shield, blue-light and UV-light filters, ability to tilt the microscope off-axis such that coaxial light is focused adjacent to the fovea).1,3,4 Microscope manufacturers and the International Commission on Non-ionizing Radiation Protection (ICNIRP) recommend using the lowest light intensity possible for the shortest period of time while still maintaining optimal visualization—however, the recommended safe exposure times are noted to be considerably shorter than the length of time for typical cataract surgery (~1.1-3.7 minutes at 50% light intensity!).1-3,6
By utilizing the 3-dimensional (3D) visualization system, in addition to increased overall visualization, the surgeon and patient are also afforded a safe and successful operative experience while being able to use significantly lower levels of illumination, without visualization compromise.1-7 Lower levels of illumination can allow for faster postoperative visual recovery and potential for less phototoxicity.1-4
Previously used mainly by
vitreoretinal surgeons, 3D, heads-up surgery has proven its utility in anterior segment surgery—both for cataract surgery, as well as
minimally invasive glaucoma surgery (MIGS).
1-7 Other studies have demonstrated similar safety profiles between ‘traditional’ and 3D approaches, as well as surgical times.
1,6,7 The benefits of a larger display that can be titrated to the surgeon, with less time spent focusing in and out of the surgical field, provides a simplified, more efficient operative environment.
1-3,6,7Below I highlight the basic principles of 3D anterior segment surgery, OR set up, and additional benefits of this exciting technology.
Basic principles and how 3D cataract surgery works
The most commonly utilized 3D Visualization System in the United States is the NGENUITY system (Alcon, Fort Worth TX).3,4 This system features a 3D ultra-high definition (UHD) 55-inch 4K Organic Light Emitting Diode (OLED) surgical display, 3D high dynamic range (HDR) camera, an ultra-high-speed image processor, and polarized 3D glasses, which are worn by the surgeon and surgical team.3,4 The HDR camera offers stereoscopic 3D imaging to create an immersive experience for the surgeon and everyone in the OR (including assistant surgeons, fellows, residents, nurses, technicians, anesthesiologists, and medical students).1,3,4 The camera for the 3D system can be coupled to any ophthalmic analog microscope with removable oculars.3,4 The OLED technology here is also able to create more natural colors, increase contrast to produce more vibrant images, and work without backlight.3,4 In addition, the image processing technology optimizes the 3D images in real-time, further enhancing the image intensity and providing brilliant contrast and color. This is exemplified by how well the surgeon can see fine details even in very dim light.1,3,4 Ultimately, this results in a more comfortable patient and less potential for light-induced macular toxicity.1,3
OR setup
The image on the display screen is viewed by the surgeon and others in the OR with polarized 3D glasses.1-7 It is important to have the correct distance between the OLED display and the surgeon, but optimal distance is dependent on the surgeon’s vision and stereoacuity, as well as the resolution of the 55” 4K display.3,4 The optimal viewing distance is usually between 1.3m (51”) and 1.5m (59”).3,4 Typically, the patient is positioned between the surgeon and display as shown in Figures 1 and 2.
Figure 1. Typical OR set up for 3D cataract surgery
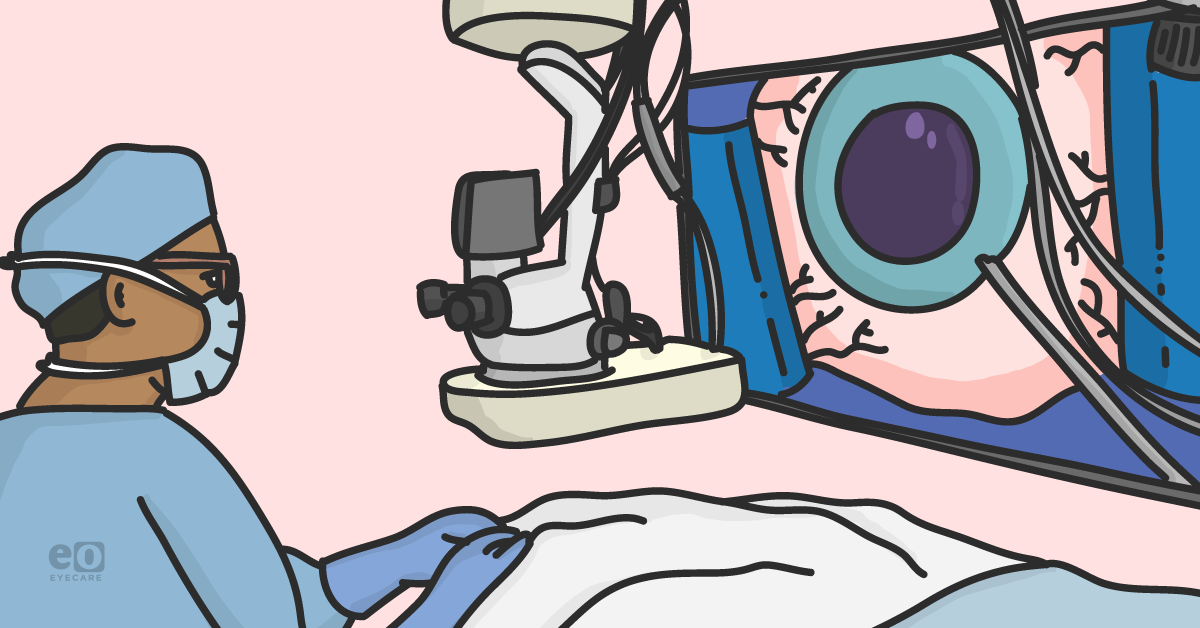
Figure 2. View from the surgeon’s perspective of the 3D heads-up display.
The OR as a “team with the same view”
As everyone in the OR has the ability to see “through the surgeon’s eyes” by using this 3D platform, there is an enhanced educational environment for
surgeons in training and OR staff.
1-4,6 It is also helpful for surgical assistants—with the assistant viewing the same images as the surgeon, the next surgical steps are more easily anticipated and correct surgical instruments can be prepared and handed to the surgeon. This produces a more efficient workflow and potential benefits to surgical performance, as well as to patient safety.
1-4,6About that view!
The NGENUITY platform allows for up to up to 5 times extended depth of field, 48% increased magnification, and 42% finer stereopsis when compared to analog microscopes.2-4,6,7 Image clarity under high magnification can aid the surgeon in visualizing fine details (think: angle structures in MIGS), as well as surgical instrument placement without losing image sharpness.1-4,6,7 In addition, the need for refocusing due to slight patient movement of lack of depth of focus is much less of an issue with the NGENUITY 3D system versus the standard operative microscope.3,4,6
Additionally, lighting is optimized across a broad range of brightness and darkness; this enables the surgeon to visualize structures of varying brightness equally and may aid in the more precise movement of instruments and more accurate manipulation of tissue.2-7
Less light intensity
Through Digital Illumination Modulation, the 3D NGENUITY system can enable the surgeon to operate at lower levels of illumination while maintaining brilliant 3D images on the screen.1,3,4 Since the image quality remains vivid, the surgeon may not even notice the difference in light intensity!1,3,4
Ergonomics
There have been several reports estimating between 46-70% of ophthalmologists experience neck or back pain, with a smaller subset denoting limited work due to pain.3,4,6 Digitally-assisted 3D surgery allows a physiologically and ergonomically optimal position for each individual surgeon.4,6 While the operating microscope has thus far proven to be the gold standard for ophthalmic surgery, it may predispose users to potential musculoskeletal issues due to unnatural ergonomics.4,6 When viewing images on the OLED screen with 3D glasses, the need for microscope oculars is obviated. The surgeon’s eyes are not required to be in close proximity to the microscope, thereby potentially relieving cervical spine fatigue from maintaining an unnatural “leaning in” position during the entire procedure.4,6
Conclusions
With studies proving equivalency between traditional operating microscope-based surgery and 3D anterior segment surgery both in operative time and low complication rate, 3D surgery brings additional features not before available as well.1-7 Digitally assisted anterior segment surgery provides the surgeon with improved images under high magnification, extended depth of field, and options for digitally enhancing images.1-7 This can provide an unparalleled level of contrast, clarity, and color.1-7 In addition, light intensity can be significantly reduced without compromising red-reflex or operability, therefore decreasing the risk of microscope-induced maculopathy.1-7
References
- Rosenberg R, Nuzbrokh Y, Sippel K. Efficacy of 3D digital visualization in minimizing coaxial illumination and phototoxic potential in cataract surgery: pilot study. Journal of Cataract and Refractive Surgery. 2021: 47(3); 291-296
- Qian Z, Wang H, Fan H, Lin D, Li W. Three-dimensional digital visualization of phacoemulsification and intraocular lens implantation. Indian J Ophthalmol. 2019; 68(3): 341-343
- Rosenberg E and Mohinder M (2021). Digitally Assisted Anterior Segment Surgery [White paper] Alcon Science. https://us.alconscience.com/sites/g/files/rbvwei1736/files/pdf/Digitally-Assisted-Anterior-Segment-Surgery-US-NGU-2000076.pdf
- Castillo G. (2021) Reaping the Benefits of Digitally Assisted Vitreoretinal Surgery [White paper] Alcon Science. https://us.alconscience.com/node/441/
- Adam M, Thornton S, Regillo C, Park C, Ho A, Hsu J. Minimal endoillumination levels and display luminous emittance during three-dimensional heads-up vitreoretinal surgery. Retina. 2017; 37(9): 1746-1749
- Weinstock RJ, Diakonis VF, Schwartz AJ, Weinstock AJ. Heads-up cataract surgery: complication rates, surgical duration, and comparison with traditional microscopes. J Refract Surg. 2019;35(5):318–322. doi:10.3928/1081597X-20190410-02
- Ohno H. Utility of Three-Dimensional Heads-Up Surgery in Cataract and Minimally Invasive Glaucoma Surgeries. Clinical Ophthalmology. 2019: 13; 2071-207